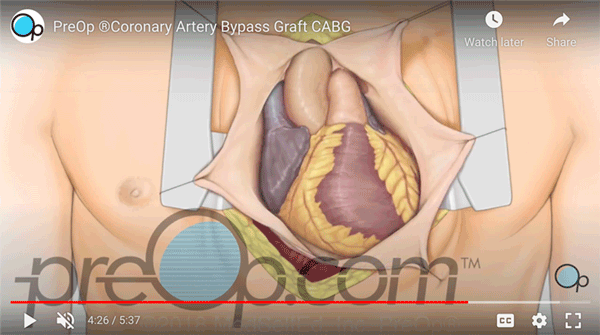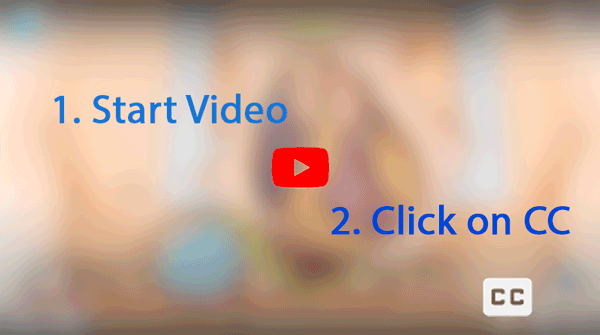
Why is a TURBT – Transurethral Resection Of Bladder Tumor done?
Your surgeon has recommended a TUR-BT to remove a tumor from the lining of your bladder. About half, or 1 in 2 bladder cancers are found early. That means the tumor is still in the lining of the bladder and hasn’t spread.
Your doctor has recommended that you have a TUR-BT or Transurethral Resection of a Bladder Tumor.
Before we talk about the procedure, let’s review some information about your body and your medical condition.
The bladder holds urine until you release it. It stretches like a balloon as it fills with urine. Muscle in the wall of the bladder works to push urine out of your body through your urethra.
Your surgeon has recommended a TUR-BT to remove a tumor from the lining of your bladder. About half, or 1 in 2 bladder cancers are found early.
That means the tumor is still in the lining of the bladder and hasn’t spread.
Bladder Cancer can be diagnosed at any age, but is most common in patients that are over 55 years old, are men, and are white
Bladder Cancer is most often linked to smoking and exposure to certain chemicals in the workplace
With a TURBT, (or Transurethral resection of bladder tumor), a surgeon uses a scope to look at the bladder lining and remove the tumor.
A scope is an instrument with a light and camera. It has a loop at the tip that can cut with heat energy.
The tumor is sent to a pathology lab for examination. Further treatment may be needed in the future, after this surgery for your cancer. These plans are made if needed after the procedure and based on the final lab results.
Now let’s talk a little more about what happens during a TUR-BT.
To start, you are given anesthesia to keep you free of pain during the procedure.
You are positioned carefully.
An instrument with a camera, called a scope, is then gently inserted into the urethra.
A numbing gel is used to help the scope glide easily.
Once the scope is inside the bladder, your doctor will fill your bladder with water or saline.
Using the fiber-optic light and camera lens of the scope to see, your surgeon will look carefully at the walls of your bladder.
The tumor is cut away from the bladder in small pieces using the loop.
Your surgeon uses suction to carefully remove those pieces from the bladder.
The loop is also used to stop any bleeding that is seen.
After the surgeon makes a final inspection of the bladder the scope is removed.
A thin soft tube called a Foley catheter may be placed in your bladder.
This tube can be used to fill your bladder with chemotherapy as part of the procedure if needed. This chemo or medication is used to prevent loose tumor cells from sticking to your bladder lining.
Sometimes the foley is left in for a few days to keep your bladder empty for healing. When it is time to be removed, the balloon is deflated and the tube easily slides out.
If your surgeon recommends chemo during the procedure, it will stay in your bladder for 1 hour. The decision depends on the size, type, and a number of tumors removed.
This medicine will not make you feel sick. You may have some bladder irritation from this.
Ask your doctor if this treatment is planned for you.
After surgery, tell someone on your care team if you have unexpected pain, dizziness or trouble breathing. You will have some discomfort but the pain should improve with medication.
After you are discharged home from surgery, you may feel well and have no problems.
Some patients will have pain with urination, bladder spasms, and frequent urination.
You may see blood and small blood clots in your urine for a few days, even in a few weeks as scabs heal in your bladder where the tumor was removed.
RIsks of the procedure are damage to the bladder, nearby tissues, infection, and bleeding.
Call your doctor if you: cannot urinate, have a fever, worsening pain, or bright red bleeding that doesn’t stop
Hospital admission, medication, or surgery may be needed to fix some complications. You may need to keep the catheter in for a longer time than expected
To avoid cancellation or complications from anesthesia or your procedure, your Job as the Patient is to not eat or drink anything after midnight, the night before surgery, not even a stick of gum
- Take only medications you were told to on the morning of surgery, with a sip of water
- Ask when to stop your aspirin or blood thinners before surgery
- Arrive on time and have a support person available
You should be ready to verify or confirm your
- list of medical problems and surgeries
- All of your medications, including vitamins and supplements
- current smoking, alcohol, and drug use
- and all allergies, especially to medications, latex, and tape
Be sure that you understand why this procedure has been recommended for you.
All surgery and anesthesia have a small risk of serious injury or very rarely death, about 1 in 100,000
If you have questions about this procedure or need further information about alternatives, ask your surgeon.
This video is intended as a tool to help you to better understand the procedure that you are scheduled to have or are considering. It is not intended to replace any discussion, decision making or advice of your surgeon.